Curriculum
The DNP Nurse Anesthesia Program is a full-time curriculum plan over 36 months (12 quarters). The first five quarters consist of didactic content delivered in a hybrid manner, blending on-campus intensive instruction with synchronous and asynchronous distance education. Part-time clinical rotations are integrated in quarters 6 – 8, gradually increasing to full-time clinical residency which occurs in quarters 9 – 12. The program confers a DNP degree upon successful completion of all program graduation requirements.
Curriculum: Didactic, Clinical, & Simulation
The Doctor of Nursing Practice in Nurse Anesthesia (NAP) Program is a full-time program delivered over 36 months (12 consecutive quarters). The first, five quarters consist of didactic content delivered in a hybrid manner, blending on-campus intensive instruction with synchronous and asynchronous web-intensive education. Part-time clinical rotations are integrated in quarters 6 – 8, gradually increasing to full-time clinical residency which occurs in quarters 9 – 12. The program confers a Doctor of Nursing Practice (DNP) degree upon successful completion of all program graduation requirements.
The DNP Nurse Anesthesia Program delivers a contemporary and evidence-based curriculum using faculty and contributors that are expert educators, clinicians, researchers, and leaders in the profession. Faculty have experience with both in-person and web-intensive education best practices and facilitate learning and professional growth with resident-centered active learning experiences, modeled clinical and scholarly excellence, and steadfast professionalism. Using a blended learning model, the curriculum combines the best aspects of distance learning activities and interactions, hands-on skills lab and high-fidelity simulation sessions, and collaborative clinical education experiences into an innovative and dynamic learning experience. Residents are trained to the full scope of nurse anesthesia practice – as well-rounded clinicians and clinical scholars. Alumni will be ready to enter full-service anesthesia delivery models upon graduation.
The South College DNP NAP is a rigorous curriculum delivered in an innovative and flexible hybrid manner. As stated above, the didactic portions of the program will be delivered via a combination of web-intensive education and in-person on-campus intensive learning sessions that are mandatory. Program faculty are both content experts and skilled in distance education pedagogy. In the majority of academic quarters, residents come together at the Parkside Learning Site in Knoxville, TN for face-to-face intensive sessions focused on instruction in complex lecture topics/skills labs/simulation training. Importantly, it will not be required for residents to physically relocate for the first year of study.
PROGRAM OUTCOMES
The NAP program outcomes are geared toward all the essential competencies needed for the doctorally prepared advanced practice nurse (APRN) specializing in nurse anesthesiology. As patient needs have become ever more diverse and complex, the skills and knowledge of APRNs are essential in providing high-quality comprehensive patient care, including along the spectrum of peri-anesthesia care. The American Association of Colleges of Nursing (AACN) has established the core competencies which meet the established essentials of doctoral nursing practice, upon which our curriculum is founded.
Additionally, the Graduate Standards set by the Council on Accreditation of Nurse Anesthesia Educational Programs (COA) are a complimentary set of didactic and clinical core competencies that serve as terminal program outcomes residents must attain prior to graduation.
DNP Program Outcomes
- Synthesize scientific evidence and methods to design, direct, and evaluate strategies to promote and provide effective patient-centered care.
- Incorporate leadership skills and interprofessional team building strategies to improve quality metrics within healthcare systems, organizations, and diverse practice settings.
- Employ information systems and technology in the delivery of transformative
- Advocate for evidence-based health policy to improve local, national, and/or global patient and health population outcomes.
- Utilize effective interprofessional communication and collaborative skills to facilitate improvement in population health.
- Apply advanced levels of clinical judgment and systems thinking in designing, delivering, and evaluating evidence-based care for clinical treatment, clinical prevention, and improvement of population health.
SAMPLE CURRICULUM PLAN
The NAP has an academic calendar unique to the program needs. Didactic courses are 11 weeks in length, inclusive of any intensive sessions. During the front-loaded didactic phase of the program (quarters 1 – 5), there will be two-week breaks between each quarter. Clinical courses are 12 weeks long. During quarters that have both didactic and clinical courses (quarters 6 – 12), all courses will start on the same date, but didactic courses will end one week earlier than clinical courses. During the clinical phase of the curriculum, there will be one-week breaks observed between each quarter.
The curriculum dashboard below displays a sample curriculum plan across the entire three years of the program. A new cohort matriculates annually in January to begin the Winter Quarter. Courses in red font are didactic courses. Courses in black font are didactic courses with an on-campus intensive session associated with the course. Intensive sessions typically consist of 5 days on campus with in-person instruction via lecture, problem-based learning, skills training, and high-fidelity simulation. Courses in blue font are clinical courses.
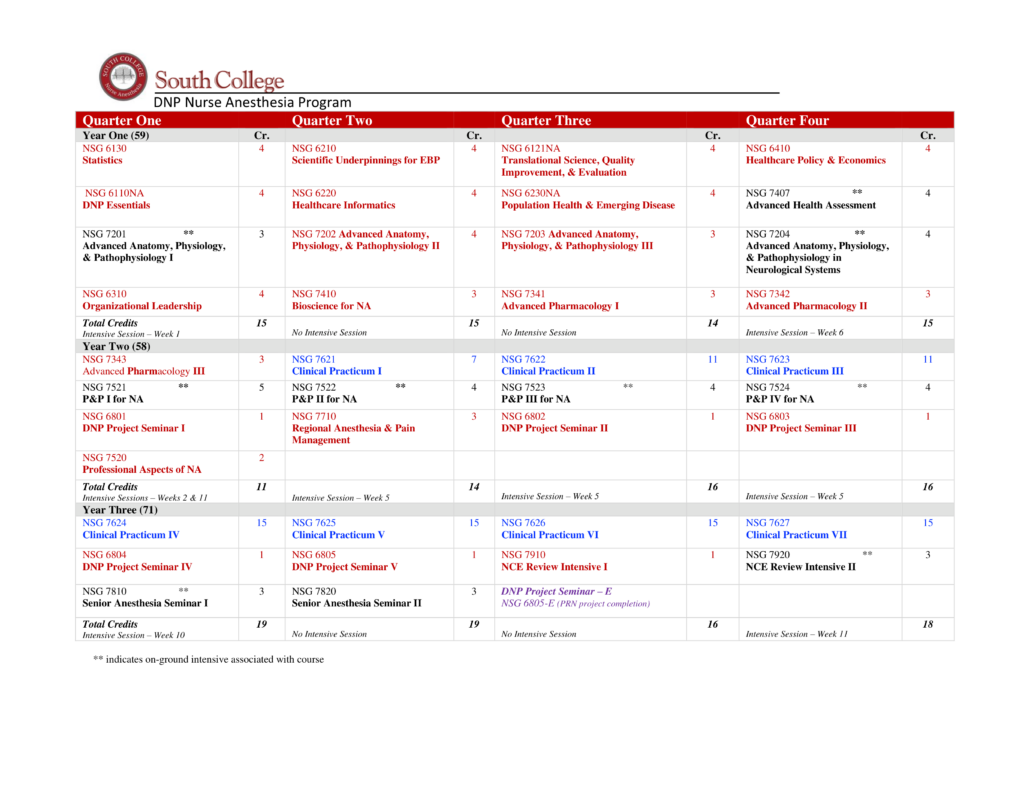
ON-CAMPUS INTENSIVE SESSIONS
On-campus intensive sessions provide opportunities for in-person didactic and simulation lab learning, as well as integration of orientation sessions, 1:1 advising sessions, collaboration with classmates on scholarly projects, peer mentoring, interprofessional activities with other South College students and faculty, and various other opportunities. The focus of our simulation curriculum is on innovation, with an emphasis placed on integrating advances within the profession of nurse anesthesiology whenever possible.
CLINICAL CURRICULUM
Clinical education occurs in regional clinical satellite campuses, distributed nationally. Rotations will be designed so that within each regional clinical satellite, a resident can acquire the entire spectrum of case minimums needed for graduation and board eligibility. Clinical education at South College provides residents with exposure to a variety of anesthesia practice settings and a wide range of patient populations across the lifespan. Clinical practicum courses begin during program year two (quarters 6-8) in a part-time capacity and increase to full-time clinical immersion during program year three (quarters 9-12). Throughout the clinical practicum series, residents are integrated into clinical settings as they learn to function as doctoral prepared certified registered nurse anesthetists (CRNAs) and deliver holistic, evidence-based anesthesia care.
Clinical education experiences provide residents the opportunity to apply their knowledge and skills through anesthesia care delivery under the direct supervision and guidance of credentialed clinical preceptors. In clinical learning environments, residents develop safe and effective skills in all aspects of anesthesia care while also developing the ability to work as part of, and lead, a healthcare team.
CLINICAL SATELLITE LOCATIONS
The South College DNP Nurse Anesthesia Program maintains exceptional relationships with clinical affiliate facilities across the nation. Clinical satellite locations include:
- Arizona (Phoenix/Tucson)
- Connecticut (Hartford)
- Georgia (Augusta)
- Florida (Orlando)
- Indiana (Fort Wayne)
- Louisiana (Alexandria)
- Maine (Bangor)
- Ohio (Cincinnati)
- Ohio (Dayton)
- Tennessee (Knoxville)
- Texas (Corpus Christi)
- Texas (McAllen/Edinburg)
- West Virginia (Huntington)
WHAT MAKES OUR CLINICAL EDUCATION PROGRAM DIFFERENT?
South College has cultivated relationships with clinical affiliate facilities across the country to meet the need of communities. Upon acceptance to the program, each resident will be assigned to a clinical satellite location based on applicant preference and availability. Our goal, if desired by the applicant, is to assign clinical rotations close to their home location to circumvent the need for relocation for the entirety of the program. Relocation will be required by the beginning of program year two if the resident lives outside of the clinical satellite location to which they are assigned. No relocation is required for the first year of the program.
Our clinical satellite campuses are situated around the nation at facilities that are invested in mentoring the next generation of CRNAs. With our hybrid curriculum design, more residents will be able to remain in their local communities while enjoying the benefits of a rigorous didactic, simulation, and clinical curriculum.
Clinical faculty are an integral part of our clinical training experiences for residents. We invest in those faculty by offering mentorship and training opportunities annually and as needed to support our clinical affiliates, site coordinators, and clinical preceptors.
It should be noted by the applicant that we will provide the clinical schedule that affords our residents the most valuable, rich, and true-to-life experiences, to mirror what life will be like as a graduate nurse anesthetist. This will include clinical rotations shifts of varied length and during off-hours. Call shifts and/or weekend hours will be incorporated into the senior level full-time clinical nurse anesthesia residency.
